Berkeley Engineering takes on COVID-19
Just weeks after COVID-19 first grabbed headlines, Berkeley Engineering researchers had pivoted their research to help test, treat and heal the growing numbers of patients. Many of our engineering makerspaces — like the Jacobs Institute for Design Innovation and the CITRIS Invention Lab — remained open and operating even during the initial shutdown to allow researchers to make products and prototypes. Here are just a few examples of how Berkeley engineers answered the call.
Breathing new purpose into sleep apnea machines
As the coronavirus began spreading across the United States, it became clear that there would soon be a high demand for respiratory devices. That’s when Bryan Martel (B.S.’86, M.S.’89 ME) got the idea to convert consumer sleep apnea devices to help COVID-19 patients with mild to moderate respiratory symptoms, saving ventilators for ICU patients.
 Dean Tsu-Jae King Liu connected him with associate professor of mechanical engineering Grace O’Connell, who quickly formed a team of student volunteers to launch the PreVENT project. The team developed designs with the help of Martel, Ajay Dharia (B.S.’04 BioE) and the late Bertram Lubin. After partnering with a UCSF clinical team — led by Aenor Sawyer and including Brian Daniel, David Harrison and Michael Matthay — the design was further refined and tested on a lung simulator. The collaboration resulted in a low-cost noninvasive ventilation system that can benefit many patients with acute infectious respiratory illnesses. The converted device uses a special face mask and a two-HEPA filter system to safely deliver oxygenated air without risking aerosolization and virus spread. Because these sleep apnea machines have already been approved by the FDA to help increase oxygen flow, and the parts used to adapt the machine are also FDA-approved, the modified machines can be deployed quickly. Access to ventilatory support has since increased in the United States, so the PreVENT respiratory devices are now being provided to other countries — including Ecuador and Malawi — that are facing shortages.
Dean Tsu-Jae King Liu connected him with associate professor of mechanical engineering Grace O’Connell, who quickly formed a team of student volunteers to launch the PreVENT project. The team developed designs with the help of Martel, Ajay Dharia (B.S.’04 BioE) and the late Bertram Lubin. After partnering with a UCSF clinical team — led by Aenor Sawyer and including Brian Daniel, David Harrison and Michael Matthay — the design was further refined and tested on a lung simulator. The collaboration resulted in a low-cost noninvasive ventilation system that can benefit many patients with acute infectious respiratory illnesses. The converted device uses a special face mask and a two-HEPA filter system to safely deliver oxygenated air without risking aerosolization and virus spread. Because these sleep apnea machines have already been approved by the FDA to help increase oxygen flow, and the parts used to adapt the machine are also FDA-approved, the modified machines can be deployed quickly. Access to ventilatory support has since increased in the United States, so the PreVENT respiratory devices are now being provided to other countries — including Ecuador and Malawi — that are facing shortages.
How wastewater can provide clues
Testing, tracing and tracking — for months, we’ve been hearing about the need for these measures to help contain the pandemic, but they’ve largely been focused on individual testing and hospital admissions. Such data can’t detect trends in the virus’s spread among the greater population, including people who are asymptomatic. Kara Nelson, professor of civil and environmental engineering, has been trying to change that. She is leading a multidisciplinary group of researchers who are working with Bay Area wastewater agencies and public health officials to develop a regional monitoring effort that accurately tracks COVID-19 in the Bay Area. By measuring levels of the SARS-CoV-2 virus in wastewater, Nelson’s team will track the virus among many thousands of people by testing a sample from a single collection station. The results will provide insight into trends in viral prevalence, determine which strains of the virus are present in a given community and identify new strains that are being introduced from other regions due to increased contact and travel. Health authorities and decision-makers will pair wastewater analysis with clinical data to provide a more complete picture that can inform efforts to control the spread of COVID-19. The detection of new strains will also help identify novel pathogens that may threaten to cause future epidemics.
When fake virus news goes viral
Misinformation via social media? We’re familiar with the dangers. But false news about the coronavirus pandemic could actually lead to increases in death. Just ask Hany Farid, professor of electrical engineering and computer sciences and at the School of Information, who conducts research on how to spot fake news, images and videos. Farid’s team launched a major survey of more than 3,000 people in the United States, Western Europe, South America, Northern Africa and the Middle East to determine how far COVID-19 misinformation has penetrated the global population. Preliminary survey information suggests that a vast majority of people believe that humans deliberately created the virus, even though scientists confirm the pathogen occurred naturally. Other myths posit that Black people are immune to the virus, the Chinese military deliberately engineered COVID-19 and drinking bleach can stop its spread. Farid and his team are trying to develop a “vaccine” to quickly counter the misinformation before it can do serious damage. They’re working with the university’s Human Rights Center to identify people and institutions who can quickly and credibly push back against misinformation, and they hope to develop strategies on stopping fake news about COVID-19 before it settles into people’s minds.
 Testing the tests
Testing the tests
Antibody testing for COVID-19 helps us understand who has been exposed to the coronavirus, how our immune systems respond and how the pandemic is spreading. But are some tests working better than others? This past spring, a collaboration between UC Berkeley and UCSF evaluated some of the more than 120 antibody test kits to provide the performance data needed to decide which tests to employ and to understand how reliable the results are. Patrick Hsu, assistant professor of bioengineering at Berkeley, led the effort with Alex Marson, associate professor of microbiology and immunology at UCSF; Caryn Bern, professor of epidemiology and biostatistics at UCSF; and Jeffrey Whitman, a clinical fellow in pathology at UCSF and a resident in laboratory medicine. In head-to-head comparisons of a dozen tests against roughly 300 patient blood samples, the researchers found that many performed reasonably well, especially two weeks or more after infection, when antibody levels begin to peak. But many other tests had false positive rates that may have exceeded the proportion of people who have been infected in some communities. The resulting paper, now published in Nature Biotechnology, is one of the first systematic studies of COVID-19 rapid antibody tests.
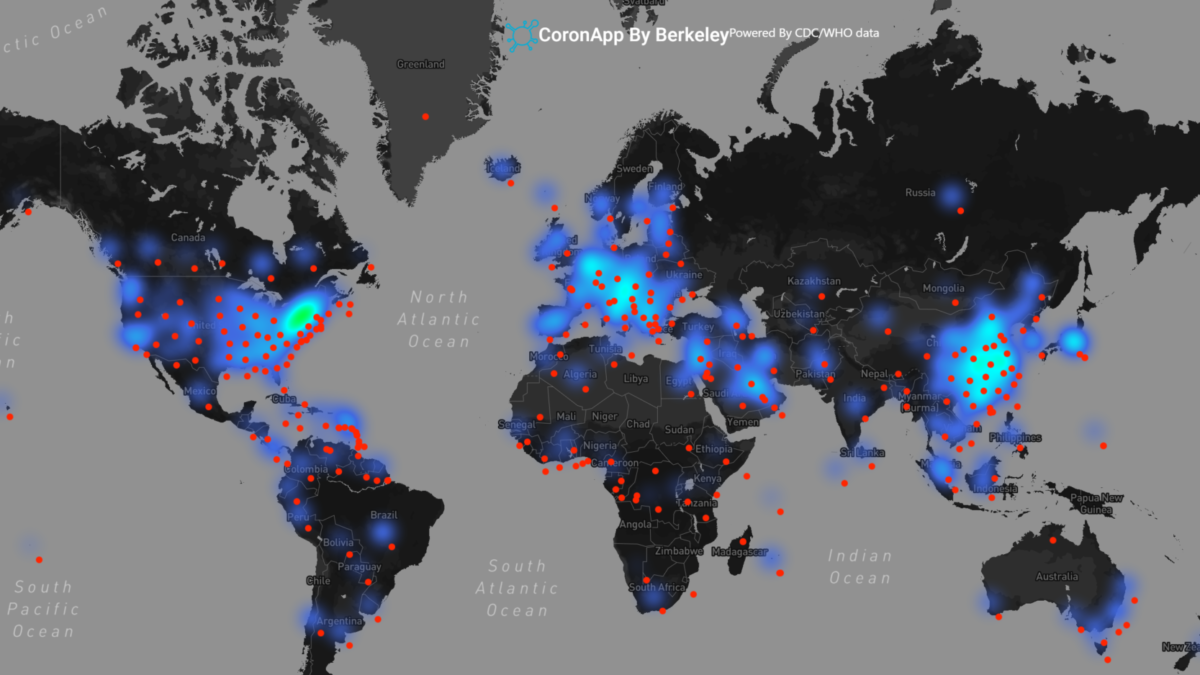
Visualizing COVID’s spread in real time
As the virus has taken hold across the country, it has become critical to have real-time tracking of infections and deaths to forecast the pandemic’s spread and severity for individual counties. Bin Yu, professor of electrical engineering and computer sciences and of statistics, and her lab have developed interpretable models that are updated daily and have curated the data to predict the trajectory of COVID-19-related deaths. Their website, covidseverity.com, gives access to those predictions in the form of interactive visualizations. They have also created a web page for hospital-level prediction, where users can upload data for a specific hospital and download prediction results for it. The uploaded data is only temporarily used for prediction and is not collected for future use.