Of mice and livers

PRIZEWORTHY: Alice A. Chen (B.S.’03 BioE) has developed a humanized mouse with a tissue-engineered human liver, which could bring about more efficient, less expensive and safer drug trials. It may also lead to a new model for studying liver diseases—such as malaria and hepatitis C—that afflict humans. (Photo by ©Andy Ryan.)
Humans and mice have more in common than just an affinity for cheese. The two mammals share about 99 percent of their genes, making mice a useful model for studying human health and disease.
There are, however, stark differences between their livers, the organ that removes metabolized drugs from the blood. When it comes to drug trials, this can create problems, as testing on mice often fails to accurately show a drug’s toxicity to humans. In clinical trials on humans, over 90 percent of drugs will fail, often due to toxicities that weren’t predicted in earlier testing. This can make the drug testing process costly and lengthy, as well as potentially dangerous to human participants in clinical trials.
But Alice A. Chen (B.S.’03 BioE) has devised a technology that could result in faster, safer and more efficient drug development. She has created a humanized mouse with a tissue-engineered human liver, allowing researchers to predict how a new drug could affect humans at a much earlier point in the development process.
A biomedical engineer and graduate student in a joint program in biomedical engineering at Harvard and MIT, Chen, 29, was recently named the winner of this year’s prestigious Lemelson-MIT Student Prize for her groundbreaking work.
“Alice Chen’s inventive accomplishments will impact the effectiveness of new therapies,” says Joshua Schuler, executive director of the Lemelson-MIT program. “Her passion to tackle problems and create solutions through collaboration and tenacity are qualities that must be celebrated at the collegiate level.”
Chen’s achievement came about as part of her thesis work, which took six years to complete. Her research included several innovations that ultimately lead to the development of a fully functioning engineered human liver implant, which could be successfully implanted and integrated into a mouse.
“I originally wanted to develop implantable livers as therapeutic devices to help treat patients with liver disease,” she says, “but I was so excited to learn that mice humanized with implantable livers could potentially translate to faster and safer medications for patients.”
Creating the human liver implant entails providing human hepatocytes (the cells that make up the main tissue of the liver) and other liver cells and chemistries that mimic the liver’s extracellular matrix. To house and deliver the hepatocytes along with these elements, she embeds them into a synthetic polymer scaffold, which is a Jello-like structural support. She then leaves the mixture to assemble liver-like processes and function on its own.
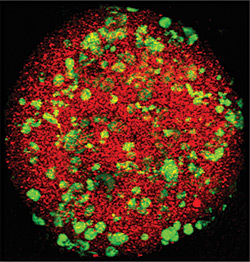
CLOSE-UP: A confocal image of engineered liver tissue (red) embedded with living cells (green). (Photo by Alice Chen/Gregory Underhill.)
The resulting implant looks nothing like an actual human liver and is similar in size, shape and appearance to a contact lens. It takes Chen just a few hours to fabricate dozens of implants, then an additional week for each implant to develop fully.
The liver can then be surgically implanted into a healthy mouse, which still retains its own liver. Because the implants can be engineered as small as micrometer-sized, multiple livers can be implanted into one mouse. “Each of these livers could be derived from different patient samples,” Chen says, “making [studies of] the mouse more informative and more efficient.”
In addition to improving drug testing, Chen’s innovation may also lead to new ways of studying human liver biology and diseases, such as malaria and hepatitis C. Research on these diseases has been challenging, as neither malady exists in rodents, but now scientists may be able to understand them better by studying them in mice with tissue-engineered human livers.
Chen believes that there is no limit to this technology, which could potentially lead to similar tissue engineered organs—such as hearts or kidneys—that could be implanted into mice, or possibly artificial livers or other organs that could be transplanted into humans.
For now, she is still exploring the best way to scale up this technology and develop it for the market. She may launch a new start-up with her adviser and mentor, MIT professor Sangeeta Bhatia, to commercialize this technology.
In the meantime, having received her doctorate in March, Chen is already hard at work as the co-founder and acting chief scientific officer of one such biomedical company, Sienna Labs. The company has developed a breakthrough class of new medical pigments that could improve the precision of microsurgeries for skin disease.
“My overall career goals are to make innovations that will improve human health and society,” she says. “I find that incredibly motivating.”
